Four years ago, Christina turner, like most Canadians, had never heard of glioblastoma. In March 2013, her husband Adam was diagnosed with this devastating cancer, which originates in the brain and is considered unbeatable.
The family was packing for a March break vacation, recalls Christina, “and suddenly Adam could barely walk. His whole left side wouldn’t function.”
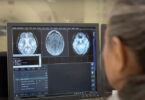
She called 911 and accompanied him to a local hospital. “Within an hour, the CT scan was done and the ER physician told me he had a lesion on the brain,” she says. “I know now that ‘lesion’ sometimes means ‘tumour.’”
Then Adam had an MRI. “At midnight,” says Christina, “I was told, ‘He’s got glioblastoma and he’s going to die from this. You need to know. Your husband is going to die.’”
A biopsy had confirmed glioblastoma. “It was quite advanced by the time he was diagnosed,” she says. “At the time, they estimated he would have 18 to 24 months.”
Glioblastoma invades the brain quickly and lethally, striking about 1,000 Canadians every year. It’s the most common and most aggressive of malignant tumours that originate in the brain.
Most patients survive less than two years following diagnosis, and the median survival rate is generally 15 months. The average five-year survival rate is 10 per cent.
“The minute they told me, I just burst into tears,” Christina remembers. “I’d lost an aunt and uncle to different types of brain tumours. I knew what the path was going to be.”
At the same time, she couldn’t believe what was happening.
“Adam was so vibrant and healthy. He was the guy who never got sick. He was a picture of health. He ate well, he worked out.”

Christina Turner (pictured with her children) lost her husband, Adam, to glioblastoma in 2013. (Photo supplied by Christina Turner)
So far, researchers have found that hereditary factors may be implicated in a very small number of patients with glioblastoma. But for most cases, there is no explanation for the cause.
What is known is that the tumour originates in the brain’s supportive tissue, or glia – a tentacled network with its own rich blood supply, making it a prime environment for a rapidly growing and highly invasive malignant tumour.
After being diagnosed with glioblastoma, Adam was transferred to Sunnybrook and into the care of internationally recognized glioblastoma specialists, neuro-oncologist Dr. James Perry and radiation oncologist Dr. Arjun Sahgal and their teams at the Odette Cancer Centre.
Currently, glioblastoma is treated with some combination of surgery to remove accessible tumours, with radiation therapy and with chemotherapy. But this cancer is a devious, elusive and deadly shape-shifter, making treatment difficult and outcomes poor.
Adam Turner died just nine months after his diagnosis, exactly one month after his 46th birthday, leaving his wife Christina and their three children, and a close-knit circle of family and friends.
Understanding the unstable glioblastoma
Unlike some other cancers where the cells are clones of each other, when one glioblastoma cell becomes two, the offspring cells don’t look like the parent.
“Glioblastoma is highly genetically unstable, more so than most cancers,” Dr. Perry points out. “Tumour cells in glioblastoma bear no resemblance to each other. We call this tumour heterogeneity, and this poses one of the biggest obstacles to successful treatment because the cells have different DNA mutations.”

A scan of the brain reveals a large enhancing mass in the brain, which causes pressure leading to headaches, nausea and vomiting and an inability to walk properly. After surgery the diagnosis was a glioblastoma.
The offspring of an entire family of glioblastoma tumour cells are all different, with different DNA machinery and different switches.
“Some of these cells respond to treatment, but some don’t, and begin to take over the tumour,” Dr. Perry explains.
That’s what makes treating glioblastoma such a challenge.
As one of North America’s most extensive practices dealing with glioblastoma and other brain cancers, Sunnybrook’s Odette Cancer Centre is, notes Dr. Perry, involved in “research embedded in care.”
The complex, challenging care provided at Sunnybrook for people with glioblastoma combines cutting-edge research and technology, clinical trials and innovative therapies and advances in precision medicine.
The goal, says Dr. Perry, is “to deliver an effective therapy without collateral damage.”
Getting inside the brain
There’s the problem of where glioblastoma is located in the brain.
Researchers have mapped areas of the brain, for example, locations linked to vision and speech. “But with glioblastoma,” says Dr. Sahgal, “everything shifts around to accommodate the tumour and there is only so much you can see with a traditional MRI.”
The neurosurgeon may think she’s cutting into a safe area, but without guided imaging that provides a map of the brain, she may be damaging critical normal tissue.
Doctors need new and better ways to see the tumour in the brain.
New technology – such as Sunnybrook’s new MR-Linac, which gives visual access to the tumour during radiation treatment and provides more advanced monitoring of the tumour as well as normal tissue during those treatments – is improving understanding of the “biomarkers of response” according to Dr. Sahgal.
“In other words, detecting and understanding the unique signals through the MR images during treatment may provide for treatments that are personalized to the patient’s unique tumour biology,” says Dr. Sahgal.
“The MR-Linac has major potential to advance the entire field of radiation response for these tumours and a new field of research,” he adds.

Researchers like radiation oncologist Dr. Stanley Liu are studying biomarkers to provide information about how well tumours will respond to radiation. (Photograph by Kevin Van Paassen)
Meanwhile, drug therapies directed at the brain must get past the blood-brain barrier – the membrane that prevents many substances in the blood from passing into the brain and nervous system.
However, Dr. Perry is excited about an innovative new ultrasound technique – transcranial focused ultrasound – that’s making holes in the brain’s fortress.
Ultrasound energy at low intensity can temporarily loosen the barrier to allow drugs through to attack the glioblastoma tumour.
“We’re in early days of a clinical trial,” says Dr. Perry, “but low intensity focused ultrasound works beautifully and it appears to be safe.”
Getting to the bottom of the genes
[mks_pullquote align=”right” width=”300″ size=”18″ bg_color=”#fff” txt_color=”#000″]
“There are things that are happening now that are so much safer that the quality of life is better for patients,” says Dr. James Perry, neuro-oncologist at Sunnybrook.
[/mks_pullquote]
Researchers have been exploring genetic mutations and biomarkers – signs of biological properties or molecules – associated with glioblastoma.
These advances in genomics are also making a difference in the treatment of glioblastoma, providing more information about which tissue and tumours will be more sensitive to radiation therapy.
That has led to the new field of radiogenomics, says Dr. Sahgal, which correlates cancer imaging features and genetic information.
Also, genomic research has made it possible, Dr. Perry continues, “to break down the vast majority of glioblastoma [cases] into four major types and to focus drug development and strategies on each of those four types” – instead of on an infinite number.
“Despite the lack of obvious new medications and therapies, there are things happening now that are so much safer that the quality of life is better for patients,” he adds. “And we’re able to be more aggressive, which is why we’re getting the gains in survival.”

Radiation oncologist Dr. Arjun Sahgal, left, and neuro-oncologist Dr. James Perry. (Photograph by Doug Nicholson)
While research continues into the molecular makeup of glioblastoma and how it can be targeted by using the body’s own immune system (immunotherapy) and other new approaches to bring about long-term remission and possibly a cure, the current goal is to prolong both the length and quality of life for patients.
“When we’re talking about glioblastoma,” says Dr. Perry, “it’s incurable. But the survival time is getting longer. Now 10 to 20 per cent of our patients survive for five years. Until the [oral chemotherapy] drug temozolomide came along, almost no one survived that long.
“We even have a patient who’s a 20-year survivor. Why did she get lucky? What is it about her tumour that’s not like the others? They appear identical. It’s all in the molecular profiling – the pathways that control the tumour. [It’s] just as random as that.
“Those of us who have been around a long time recognize that the effects of our treatment pale in comparison to the effects of the genetic lottery.”
As the research and innovation continue at Sunnybrook’s Odette Cancer Centre, Dr. Perry is hopeful about the future for glioblastoma patients.
“I think the two-to-five-year survival will continue to go up.”
Adds Dr. Sahgal, “There are very few places in the world that can do all of this.”
Learn about the Gord Downie Fund for Brain Cancer Research at Sunnybrook