Clarice Shen’s nursing shift on January 23, 2020, started like any other. As she scanned her assignments for the evening in one of Sunnybrook’s general internal medicine wards, though, she noticed it included an empty room marked as ‘closed’.
“I thought that was a bit odd to be assigned a closed bed,” says Clarice, 25, who asked her supervisor if there was some sort of issue with the room assignments.
Her supervisor explained that the room had been set aside in case a patient with a suspected case of the novel coronavirus (later named COVID-19) needed to be admitted to the hospital, since it was a negative pressure isolation room with a separate ventilation system.
“Back in January, we had only just started to hear about the novel coronavirus. No one really knew very much about it, or how to treat patients who were sick with the virus,” says Clarice.
“I remember thinking to myself, ‘what are the chances we would actually admit a patient tonight?’”
But a few hours later, her unit got a call from the Emergency Department. Clarice’s supervisor pulled her aside and relayed the news: they were admitting a patient with respiratory symptoms and a concerning chest x-ray who had just returned from Wuhan, China. He would be brought up to the isolation room on their unit and would be treated as a Person Under Investigation (PUI) until his test results came back, but they strongly suspected this could be the first confirmed case of the novel coronavirus in Canada. Clarice would be his primary nurse.
“I never felt scared. Everything just felt surreal,” says Clarice.
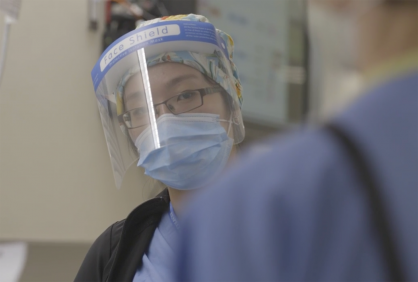
Clarice (above) was just three months into her new career as a member of Sunnybrook’s Acute Care Nursing Resource Team (ACNRT) when she volunteered to care for the patient with the first confirmed case of COVID-19 in Canada.
“I was thinking a lot about the best way to care for him, and what kind of isolation protocols would be followed. How sick will he be? What if he codes when he gets here – were there special procedures I had to follow? So many scenarios were running through my mind.”
Before the patient arrived, the hospital shift manager arrived on the unit to give Clarice a detailed refresher on donning and doffing the required personal protective equipment (PPE), as well as going over what would happen if the patient suddenly deteriorated, or “coded.”
“Everyone was very open about the fact that there was a lot about this virus we did not know. That made me feel more at ease, the fact that we were all learning about this together. I had so much support behind me from the other nurses on the unit that night,” she says.
Once the patient arrived on the unit, he was taken into the isolation room. When Clarice went in to introduce herself and explain the next steps in his care, she realized the health-care workers weren’t the only ones feeling the stress of the situation.
“It must have been terrifying for him, to have everyone in PPE and trying to stay away from him as much as possible, and to not have any family members around,” says Clarice.
Later that weekend, when the patient’s test results for the virus came back as positive, “I kept thinking about how isolated and alone he must be feeling,” she says.
She was scheduled to work three more shifts that week, so she did the thing that made the most sense to her: she called her supervisor and volunteered to care for him for the rest of the week.
“I was a familiar face to the patient, I could communicate with him in his language, and I felt comfortable with the protocols and procedures we were following. Plus, I was living alone and would not put any vulnerable members of my family at risk. Why not?”
Watch: Clarice shares her story on Cityline (and receives a big surprise!)
‘It felt as though the experiences and decisions I’d made in my life had been leading to me toward that moment’
Clarice says she was first inspired to go into nursing while growing up in Toronto during the 2003 SARS epidemic.
She remembers flipping through a copy of Reader’s Digest, trying to find the crossword puzzle, when she came across an article about nurses caring for patients who were sick with SARS.
“I thought those nurses were so courageous to do this work even though they felt scared, and some even came down with SARS themselves. That’s when I first thought that maybe I could be a nurse someday,” says Clarice.
Clarice eventually turned that idea into reality by enrolling in the Lawrence S. Bloomberg Faculty of Nursing at the University of Toronto, graduating from the program at the end of 2019.
[mks_pullquote align=”right” width=”300″ size=”18″ bg_color=”#fff” txt_color=”#000″]
“I really believe that everything aligned so that I was in the right place, at the right time , to help this patient.”
– Clarice
[/mks_pullquote]
She was just three months into her new career as a member of Sunnybrook’s Acute Care Nursing Resource Team (ACNRT) when she volunteered to care for the patient with the first confirmed case of COVID-19 in Canada.
“It felt as though the experiences and decisions I’d made in my life had been leading to me toward that moment,” says Clarice.
“SARS is what got me interested in nursing in the first place, so to finish nursing school just a few months before a new pandemic hit, and then to be working on the unit that night in January and be assigned that isolation room – I really believe that everything aligned so that I was in the right place, at the right time, to help this patient.”
While Clarice was only a few months into her new nursing role, she is no stranger to demonstrating leadership through action: she spent the last eight and a half years serving as a Primary Reservist in the Canadian Armed Forces, only leaving her position as an army corporal earlier this year at the peak of the first wave of COVID-19, when it became clear she had to prioritize her work at the hospital.
“I was 16 when I joined the military, so it was hard to make that decision to leave, but they were understanding,” says Clarice.
“They told me it was time to go and fight a different kind of war.”
‘I know this is where I want to be’
The first patient with COVID-19 was discharged home after a short hospital stay. But when the pandemic was declared two months later, Clarice once again volunteered to work in a new unit created to care for patients with COVID-19.
Clarice and some of the other ward nurses had never worked in an intensive care unit (ICU) before, so the COVID-19 unit implemented an innovative hub model to help familiarize them with the unique demands of ICU nursing.
“We were each paired with an ICU nurse, and then we would care for two patients together as a team. While some of these patients were relatively stable, others would become critically ill very quickly. It was a really challenging, eye-opening experience,” she says.
Clarice says that working on the COVID-19 unit has caused her to re-think the direction of her career. She now plans to pursue a specialized certificate in intensive care nursing in the near future.
“Before all of this, I had never really thought about being an ICU nurse, especially not so early in my nursing career. But now I know this is where I want to be,” she says.
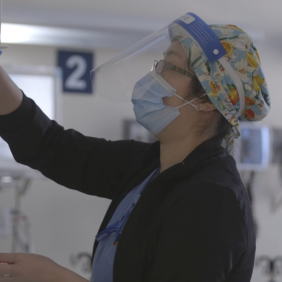
“Before all of this, I had never really thought about being an ICU nurse, especially not so early in my nursing career. But now I know this is where I want to be,” says Clarice.
Though there are fewer patients with COVID-19 in the hospital at the moment, Clarice’s shifts are busier than ever.
She says that some of her most difficult moments during the pandemic have been as a result of the ongoing restrictions and changes that all health-care workers, patients and families are trying to navigate.
“When visitors became restricted, that was very challenging for patients. We tried to fill that gap as best we could, sometimes using technology like tablets and video calls to help patients stay connected. But of course, it wasn’t really the same,” says Clarice.
“I’ve always enjoyed spending time with my patients, trying to help them understand what’s going on with their care. Sometimes it’s as simple as explaining why I’m putting a saline solution in their IV line – I try to help them feel that we’re not doing something to them, we’re doing it with them. That’s become even more important now that many patients don’t have access to their usual support systems.”
What the future holds
While the next few months hold a lot of uncertainty, Clarice does know one thing for sure: she and her fiancé, Guillaume, are finally going to get married this fall.
“He also works as a nurse at a hospital downtown, so we had to put off our wedding plans earlier this year. It will be small since there are still a lot of restrictions, but we’ve never really liked the idea of having a huge wedding anyways,” says Clarice.
“Now I just need to stop working so much overtime so that we can actually plan it!”