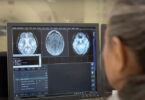
Our eyes, it has long been said, are windows to the soul. Now, new research is hoping they can also provide some insight into the link between the health of our brains and our bodies.
This is the aim of a groundbreaking study at Sunnybrook focusing on the eyes of Lauren and dozens of other youth, ages 13 to 20.
The hope is that images of the tiny blood vessels of the retina, at the back of the eye, may unlock part of the mystery about why people with bipolar disorder have a higher and earlier risk of heart disease and cognition problems.
Could it be that atypical blood flow also impacts mood and brain function? The multidisciplinary study is unique in several ways.
[mks_pullquote align=”right” width=”300″ size=”18″ bg_color=”#fff” txt_color=”#000″]
“I’m hoping that for future generations – and possibly even any children I may have – this research will really benefit them“
– Lauren, study participant
[/mks_pullquote]
It involves using a special camera to photograph the inside of the eyes of Lauren and other participants with bipolar disorder, as well as a control group without major mental illness.
It also marks the first time retinal photography has been used to capture images of the blood vessels in the eyes of young people with bipolar disorder. The researchers are also looking at factors that may predict small-vessel problems, such as inflammation, exercise, diet and use of medications.
The objective is to examine the blood vessels of the retina, which are “a close relative of the blood vessels in the brain,” notes youth psychiatrist Dr. Benjamin Goldstein, who is the director of Sunnybrook’s Centre for Youth Bipolar Disorder, the driving force behind the ongoing research.
Retinal photography has long been used in studying conditions related to aging, such as Alzheimer’s disease, atherosclerosis (hardening of the arteries) and diabetes.
“The retina offers the only way of directly visualizing central nervous system blood vessels,” explains Dr. Goldstein, who is also director of research in Sunnybrook’s Department of Psychiatry.
“Blood-vessel problems may be one of the core causes of bipolar disorder, and [retinal photography] is a very inexpensive, non-invasive way of understanding this link.”
According to Dr. Peter Kertes – Sunnybrook’s chief of ophthalmology and a member of the youth bipolar retinal photography research team – the retina, which is “essentially an extension of the brain,” works like the film in a camera. It’s responsible for interpreting what is out there in the world and sending that back to the brain as vision.
The project illustrates a unique collaboration between different specialists within Sunnybrook’s Hurvitz Brain Sciences Program, one that includes Dr. Goldstein, Dr. Kertes, Dr. Sandra Black, a senior scientist and neurologist, and Dr. Victor Yang, a neurosurgeon and medical biophysics expert.

From left: Drs. Victor Yang, Benjamin Goldstein, Sandra Black and Peter Kertes are part of a cross-departmental team involved in work linking retinal-vascular systems and bipolar disorder (Photo by Kevin Van Paassen).
“This study has brought together researchers who otherwise don’t cross paths, which is highly atypical – and inspiring from my perspective,” Dr. Goldstein adds.
“It’s been the fastest-recruited study we’ve ever had in our research program, and I think that speaks to the appeal of taking a picture of the eye to understand mental illness. These are not typically two things you pair with each other.”
Study recruitment is ongoing; the goal is to include a total of 300 subjects.
In Lauren’s family, another member has been diagnosed with bipolar disorder, her 24-year-old brother, James. Their mother, Gen, has always encouraged them to participate in research and not to feel they have to hide their diagnoses.
“I eventually told my friends [about the diagnosis],” recalls Lauren, who was 16 when she was referred to Dr. Goldstein after experiencing symptoms of bipolar disorder.
“I’m comfortable expressing myself because it’s no different than telling people you have diabetes or some other health issue.”
And she participated in several youth bipolar studies before turning 21 in the fall.
“I’m hoping that for future generations – and possibly even any children I may have – this research will really benefit them,” says Lauren, who has a graduate diploma in early childhood education and recently started her career.
The primary tool being used in the project to photograph retinas is a Topcon TRC-50DX Type IA camera in Sunnybrook’s Department of Ophthalmology.
To start, drops are administered in the eyes of each study subject, so the pupils are dilated widely enough for the camera to see into them properly.
Next, the ophthalmic photographer positions the subject to sit facing the camera lens, with their chin in a chin rest and their forehead against a bar that’s part of the apparatus.

“I’m comfortable expressing myself because it’s no different than telling people you have diabetes or some other health issue,” says Lauren of her bipolar disorder diagnosis. (Photo by Doug Nicholson)
The photographer then adjusts the exposure to the proper intensity to photograph the retinas. Lauren says the whole process took about half an hour (with the photography component taking less than a minute).
Dr. Black says one of the obstacles the researchers were working to overcome was to figure out how to actually measure the blood flow in the retina.
However, that’s where Dr. Yang’s expertise has proved important. He uses optical coherence tomography (OCT), a revolutionary medical imaging technique that captures high-resolution 3D images showing a cross-section of the retina and all of its layers.
“It allows us to see into the body without injecting any dyes,” says Dr. Yang. “Our lab has been developing OCT technology for the past two decades and is opening up a whole new understanding of the effects of blood flow in the brain and retina.”
Notes Dr. Black, Brill Chair of Neurology, “From this melting pot of different specialties working together, new ideas can spring forth.” For his part, Dr. Kertes says, “I have learned a great deal about dementia [from another study with Dr. Black] and bipolar disease in particular, and feel confident that this insight and knowledge have made me a more caring and better doctor.
“The work that [ophthalmologists] do in restoring and preserving vision has been fantastically gratifying, but the potential of contributing to the diagnosis and monitoring of neurological and psychiatric diseases is tremendously exciting.”
Early results of the study have uncovered some interesting findings about teens with bipolar disorder, specifically the following:
-
Those with high blood pressure had poorer retinal blood-vessel health.
-
Healthy blood vessels in the body are linked to healthier blood vessels in the eyes.
-
Teens that did well in a series of specialized online games aimed at measuring their ability to problem-solve had healthier blood vessels in their eyes.
The researchers hope their work will lead to new approaches to diagnosing, monitoring and treating mental-health issues, with a focus on prevention.
For instance, they foresee a future in which blood-vessel health is considered in the diagnosis, monitoring and early treatment of bipolar disorder, and prevention and treatment approaches may include everything from prescribing exercise (to help improve blood flow in the brain and body), to using different counselling methods and medication that may not have been standard practice before.
Knowing that bipolar disorder isn’t just a mental illness can be “empowering,” notes Dr. Black, and can “motivate kids to do the right thing, which is to exercise [and] take it seriously, because you can change your outcome, and you can change your life by dealing with that biology.”
Other Sunnybrook-led studies get to the heart of youth bipolar disorder
Sunnybrook’s groundbreaking retinal photography project is just the latest of a wealth of research examining the link between youth bipolar disorder and blood-vessel and heart health.
Dr. Goldstein – director of research for the hospital’s Department of Psychiatry, as well as director of its Centre for Youth Bipolar Disorder – was also the lead author of a 2015 scientific statement published in Circulation, the American Heart Association’s Journal. The paper determined that depression and bipolar disorder increase the risk that young people will develop atherosclerosis (hardening of the arteries) and heart disease.
In late 2016, Dr. Goldstein led another study, the first to examine the link between cardiovascular health and mental flexibility in adolescents, ages 13 to 20, with bipolar disorder. The results of his research found that elevated blood levels of triglycerides (a type of fat that can be measured in the blood), which are known to increase the risk of heart disease, are also associated with decreased “executive function,” determined based on mental flexibility during a computerized task.
Earlier studies had already concluded that adults with bipolar disorder had greater cardiovascular risk factors, such as obesity, high blood pressure and high levels of blood sugar and triglycerides, compared to adults without bipolar disorder.
[mks_pullquote align=”right” width=”300″ size=”18″ bg_color=”#fff” txt_color=”#000″]
“The goal is to prevent these kids from developing heart disease in the first place.”
– Dr. Benjamin Goldstein
[/mks_pullquote]
In Dr. Goldstein’s research findings, the adolescent subjects with bipolar disorder also had greater cardiovascular risk factors and didn’t do as well on a computerized test measuring mental flexibility and impulsive risk-taking, compared to the control group.
So what’s happening with the vascular systems of teens with bipolar disorder?
“There are multiple things going on,” Dr. Goldstein points out. “These teens are similar to adults with bipolar disorder – they’re more likely to smoke, less likely to exercise, and their nutrition is not as good [as individuals without bipolar disorder]. “But it’s also stressful to live with bipolar disorder, so [the strain] impacts their risk for heart disease.
And then there’s another piece – some of the medicines used [to treat and manage mental health conditions] increase weight. All these factors are part of the story.”
“We know that the reality for middle-aged adults with bipolar disorder includes excessive heart disease which can shorten their life by 10-15 years. That’s the status quo and we’re not happy with the status quo,” Dr. Goldstein continues. “The goal is to prevent these kids from developing heart disease in the first place.”